February 4, 2024, 1:43 PM IST
What does “better safe than sorry” mean to you?
Most people believe it is safer to continue taking certain medications rather than risk slightly elevated blood pressure, blood sugar or cholesterol levels. But what if the opposite is true.
In recent years, many senior doctors have realized that we’ve swung too far towards medicating lifestyle diseases. Studies from the past two decades suggest that excessive medication can often be more harmful than no medication at all. This phenomenon is known as the J-Curve. Progressive doctors have been vocal against overmedication for controlling blood pressure, sugar, and cholesterol. As a result, guidelines for medication thresholds have been revised. However, these changes haven’t been widely disseminated, leading many doctors to follow outdated guidelines.
Later in this blog, I’ll present evidence supporting the revision of these guidelines towards more moderate medication thresholds. We’ll also delve into the politics of the pharmaceutical, food, and healthcare industries, and examine the roles government and media play in our health.
Emerging evidence shows that previous approaches were flawed and potentially more harmful. Many doctors are now reevaluating their recommendations for treatment and testing. The increased specialization in medicine often leads to tunnel vision, neglecting the overall quality of life and mortality. Furthermore, our understanding of drug interactions is limited, and prescriptions from multiple specialists can lead to Adverse Drug Reactions (ADRs). I’ll cover ADRs more in future blogs.
Human Body is Self Healing
“The human body is a remarkable self-healing mechanism, often smarter than we acknowledge. It adeptly copes with the diet and lifestyle it encounters. Elevated blood pressure, sugar, or cholesterol levels are often the body’s compensatory responses to various conditions.
However, the body struggles with synthetic medications. These substances are foreign and can disrupt the body’s natural compensatory mechanisms. Moreover, they place a strain on the liver and kidneys, affecting them in ways not fully understood.
To be safe, it’s advisable to first address diet and lifestyle changes, allowing the body to naturally adjust these health markers. Of course, always seek medical advice and discuss your preferences with your doctor.
J -CURVE Concept
It’s well-known that symptoms like high blood pressure or blood sugar are detrimental to health and, if uncontrolled, can lead to a shortened lifespan. Diseases typically follow a slanted S-curve, indicating that minor deviations from normal levels are less harmful and more manageable than more severe deviations. The impact on life expectancy isn’t linear; a slight worsening of health markers is more concerning at advanced levels. For instance, a 10% increase in systolic blood pressure from 120 to 132 is concerning, but not alarmingly so. However, a 10% rise from 140 to 154 is significantly worrying. If it jumps 10% from 190 to 209, it becomes critical and demands immediate action.
We also know that all medications have some negative side effects which may reduce our life expectancy. So clearly minimizing or eliminating medications should be a goal. Some BP patients are on a single pill which may not be as harmful, but some are on 6-7 different pills just for controlling BP. That situation is not at all desirable and if the person is also on diabetic or statin medications, it can harm in ways we do not fully understand.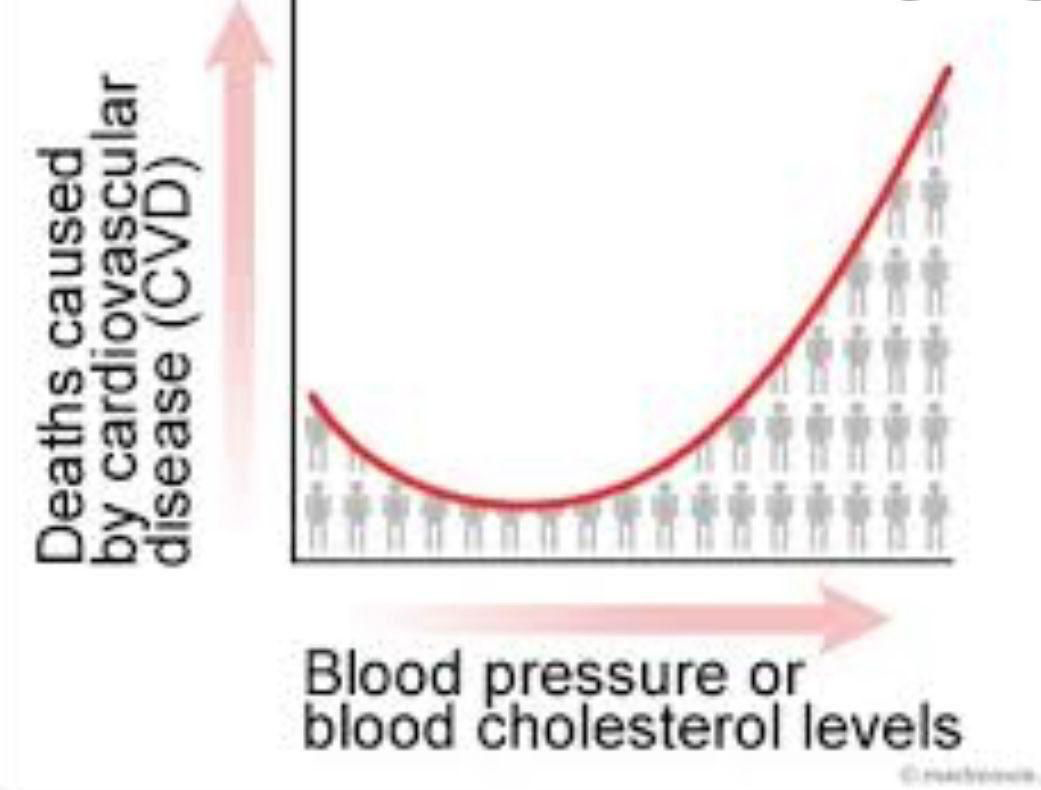
Given the considerations mentioned, many senior doctors are now questioning the wisdom of stringently controlling health markers with aggressive medication. Recent studies have been conducted to assess the impact of such medications and disease markers on overall life expectancy. These studies indicate that optimal results are often achieved with a moderate approach.
ACCORD Study
The Action to Control Cardiovascular Risk in Diabetes (ACCORD) study, initiated in September 1999 and sponsored by the National Heart, Lung, and Blood Institute, is a significant example. This study aimed to examine the effects of intensive glycemic control, blood pressure management, and multiple lipid management on major cardiovascular events (heart attack, stroke, or cardiovascular death) in patients with type 2 diabetes. The study, a landmark in its field, was supported by several collaborators:
– National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK)
- National Institute on Aging (NIA)
- National Eye Institute (NEI)
- Centers for Disease Control and Prevention
The researchers initially hoped that tighter control of blood sugar and blood pressure would enhance life expectancy. However, within eight years, it became evident that such stringent controls were, in fact, increasing all-cause mortality rates among patients. Consequently, the duration of the study was curtailed, as it would have been unethical to continue exposing patients to such risks. The chart below presents the raw data from the ACCORD study, which the American College of Physicians (ACP) used to revise their diabetes guidelines in 2018. It is noteworthy that even they took a decade to update their guidelines.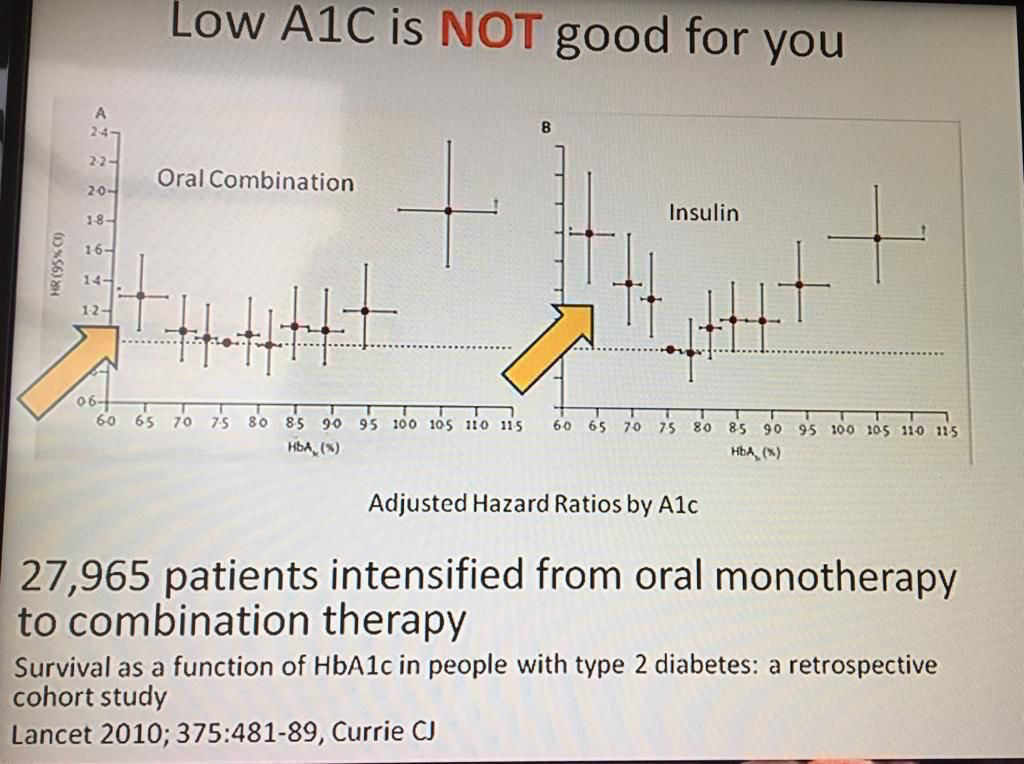
The link to their announcement of March 6, 2018 is given below.
After the ACCORD study, many doctors called for a revision of the guidelines for blood pressure and blood sugar medications. In response, the Joint National Committee on Detection, Evaluation, and Treatment of High Blood Pressure (JNC-8) revised its blood pressure control guidelines in 2014 as shown below.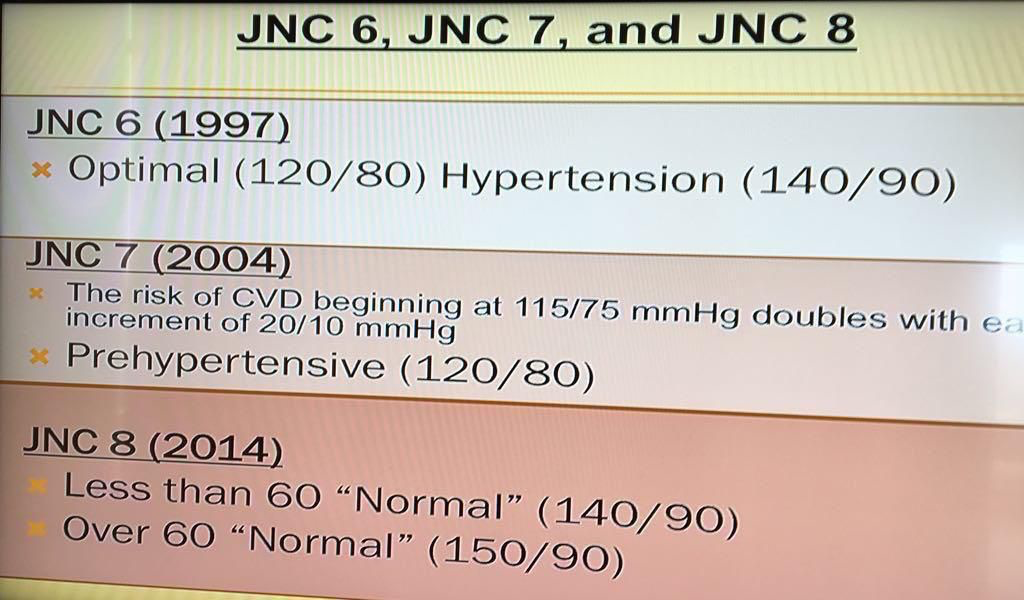
The American College of Physicians updated their diabetes guidelines in March 2018. Both revisions faced objections from those whose income was most affected. In US, the Food & Drug Administration (FDA) was pressured to disband the JNC, which had served for over four decades and transfer authority to the American Heart Association (AHA) and the American College of Cardiology (ACC).
The American College of Physicians (ACP) 2018 diabetes guideline revision alarmed the American Association of Clinical Endocrinologists (AACE) so much so that they reinstated their own, more restrictive guidelines within seven days. I will discuss these issues in more detail in the coming months under the topic of the Politics of Diet & Health. For now, my aim is to inform you about the J-Curve and why it occurs. Many of you may not be aware of these recent revisions and could be overmedicating. I recommend discussing this with your healthcare providers as soon as possible.
To Read this article on Times of India click here


Share and get 15% off!
Simply share this product on one of the following social networks and you will unlock 15% off!